- HOME
- Department
- Pelvic Organ Prolapse Center
-
Related Links
Pelvic Organ Prolapse Center
The Pelvic Organ Prolapse Center treats pelvic organ prolapse including cystocele, rectocele, and uterine prolapse in women.
What is pelvic organ prolapse?
Certain muscles and ligaments at the bottom of women’s pelvis support organs such as the uterus, bladder, and rectum. The muscles support the organs so that they do not come out of the pelvis due to abdominal pressure. When these muscles or ligaments loosen due to childbirth, obesity, or aging and the uterus, bladder, or rectum descends to the vagina, these organs come out from the vaginal opening. Prolapse of the bladder is called cystocele, prolapse of the uterus is called uterine prolapse, and prolapse of the rectum is called rectocele. Pelvic organ prolapse (POP) is a general term including cystocele, uterine prolapse, and rectocele.
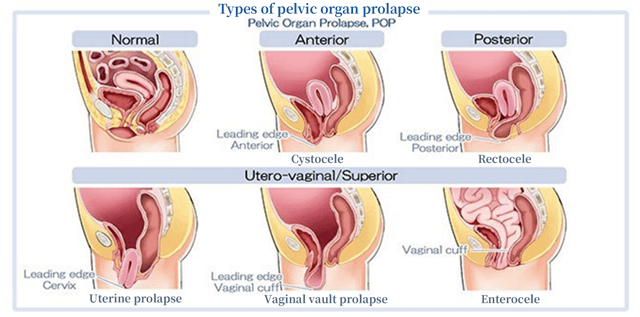
Cystocele occurs most frequently, accounting for 60% of POP. The most common cause of POP is childbirth; aging, obesity, and constipation are some other known causes.
Stage classification of POP and the target of treatment
Stage I: The most descending part is located more than 1 cm above the hymenal ring. There is no major problem in daily living at this level.
Stage II: This involves mild to moderate POP. The most descending part is located within the range of less than 1 cm above and below the hymenal ring.
Stage III: This involves moderate to severe pelvic organ prolapse. The most descending part is located at over 1 cm from the hymenal ring but not exceeding the range 2 cm shorter than the entire length of the vagina. The prolapse can be touched at the vulva, and unpleasant symptoms appear.
Stage IV: The posterior vaginal fornix (the most distal portion of the vagina) completely slips outside and the cervix is visible.
Target patients: Among patients diagnosed with POP, we will perform laparoscopic or robotic sacrocolpopexy for those with a moderate to severe condition (Stages III and IV).
■ Robotic sacrocolpopexy techniques
- The surgery is performed under general anesthesia. The anesthesiologist will explain the details of anesthesia before surgery.
-
- Make a 1–2-cm incision in the lower border of the umbilicus (sometimes the upper border) and insert a camera port. Insufflate the abdominal cavity with carbon dioxide to create a space for surgery. Additionally, insert three to four surgical ports into the lower abdomen.
-

Surgical assistant robot

- Process the ligaments and blood vessels connecting the uterus, pelvis, and ovaries, and lastly cut the cervix to remove the uterus. One ovary may be removed together depending on the surgery.
-
- Peel off the area between the vagina, bladder, and rectum to expose the levator ani muscle group. Sew a non-absorbable membrane called a mesh to this muscle. Pull up this mesh cranially and sew to the sacrum for fixation.
-
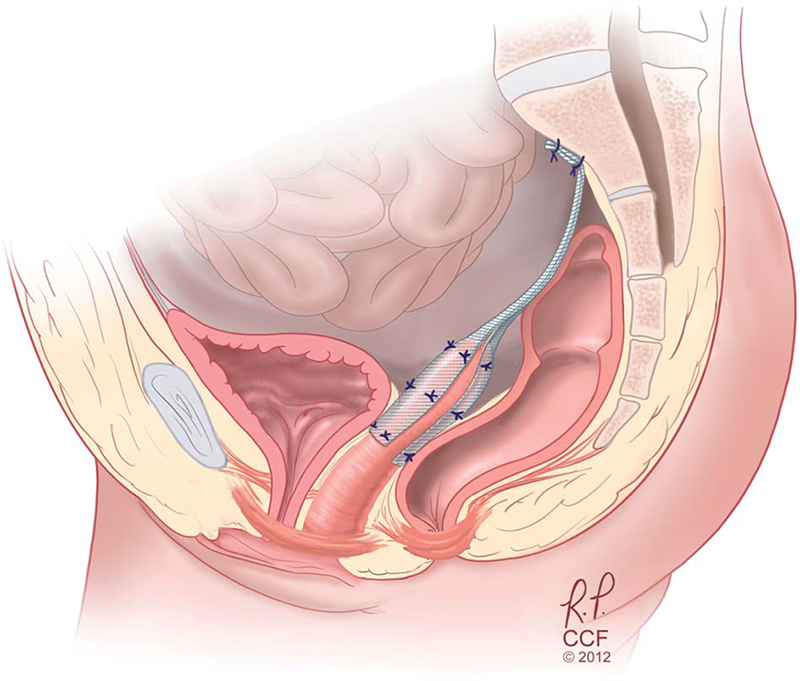
(※1)
- Remove all ports and suture the wound. There is no need for suture removal.
- (※1 Cited from Walters M. D. et al. Surgical treatment of vaginal apex prolapse. Obstetrics & Gynecology, 2013)
■ Alternative treatments
Vaginal hysterectomy + colporrhaphy/colpocleisis
It is a proven operation, but the recurrence rate is said to be 40–70%, and there is no consideration for sexual function.
Tension-free vaginal mesh surgery (TVM)
It was reported in Japan in 2006. The anterior vaginal wall is incised, and a polypropylene mesh sheet is placed between the bladder and vagina and fixed to the cervix. It has advantages, such as being a minimally invasive surgery and not impairing sexual function. The recurrence rate is about 5%. However, if the symptom recurs, TVM cannot be performed, and sacrocolpopexy is performed. Side effects caused by the mesh have been reported. These include vaginal erosion (less than 10%), dysuria (10%), urinary retention, and urinary incontinence (15%).

Ring pessary
Conservative treatment
The ring pessary is inserted into the vagina with regular monitoring in the outpatient setting. Although it has advantages, such as minimal invasiveness, detachability, and low cost, it requires regular hospital visits and frequently causes problems such as vaginal wall erosion, bleeding, increased vaginal discharge, and cystitis. Surgical therapy is necessary to fundamentally solve the problem.
Message to patients visiting the Pelvic Organ Prolapse Center
Our Center has a system in which urologists and gynecologists cooperate with each other to ensure that patients can safely undergo surgery and treatment. The degree of pelvic organ prolapse and the resulting decrease in quality of life vary from one patient to another. We put together the opinions of Urology and Gynecology and propose appropriate treatment methods. If you have been treated conservatively but your symptoms have worsened, we may be able to suggest other treatment options. Please bring a referral letter of the previous doctor and, if possible, also the most recent diagnostic imaging materials.
If you have a medicine notebook, please bring it with you. This is because bleeding may occur at the time of surgery depending on the drugs you take, such as drugs to thin your blood. At our department/center, pharmacists intervene and check the medications you are taking before surgery. If you have a medication notebook, you can smoothly receive treatment.
Masaki Nakamura, Director








