- HOME
- Department
- Artificial Joint Center
-
Related Links
Artificial Joint Center
Orthopedic Surgery at the hospital conducts specialized artificial joint replacement surgery of the hip and knee joints at the Artificial Joint Center.
Currently, the Center conducts approximately 150 artificial joint replacement surgeries per year.
The Center strives for safe treatment with minimal stress on the body based on extensive treatment experience.
Overseas, a registration system is in place for artificial joint replacement surgeries and detailed reports are being made about the long-term results.
At the department, based on these reports, we place the utmost priority on ensuring that we conduct treatment with exceptional long-term results. We strive to offer comprehensive care and treatment that each and every patient will feel is of a high quality.
- Artificial hip joint replacement surgery
- Artificial knee joint replacement surgery
- Reverse Total Shoulder Arthroplasty
Artificial Hip Joint Replacement Surgery
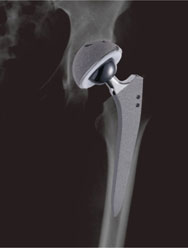
Artificial hip joint replacement surgery is a surgery where hip joints that have been damaged are replaced with artificial joints.
Artificial hip joints consist of a thigh component and acetabular (pelvis) component. Titanium alloy, ceramic, and polyethylene (plastic), which have high biocompatibility, are used as materials.
It is structured so that there is movement between the ball of the thigh component and the socket of the acetabular (pelvis) component.
Artificial hip joint replacement surgery is a suitable treatment method in cases where there is strong pain from osteoarthritis and other hip joint diseases that does not improve with treatment such as physical therapy or medication.
Artificial hip joint replacement surgery is highly effective in alleviating pain in the hip joints, and tens of thousands of people undergo the surgery every year.
Life After Surgery
The pain in your hip joints will be alleviated, and you will be able to live an active life. Once your energy recovers, you will be able to engage in moderate exercise such as cycling, golf, and hiking. In order to ensure that your artificial joints last for an extended period of time, exercise that places strong impact on the hip joint such as jogging and contact sports is not recommended.
Durability of Artificial Joints
New technologies and materials have been developed, enhancing the durability of artificial joints. 20 years after surgery, approximately 90% of patients continue to use their artificial joints. If the artificial joints become worn down or if the artificial joints and bone become loose, a repeat replacement surgery may be required to replace the artificial joints.
Preparation for Surgery
Once the date of the surgery is set, preparations begin from three to four weeks in advance.
Physical Checkup
In order to confirm that it is safe to undergo the surgery, you will be given tests such as a blood test, urine test, electrocardiography, and chest X-ray. Depending on the test results, you may be asked to undergo further testing or consult another clinical department.
Comorbidities and Medications
We will confirm the diseases for which you are being treated and any medications you are taking. Depending on the type of medication, you may need to stop taking the medication prior to surgery or adjust the dose.
Autologous Blood Deposit
There are cases where transfusion may be necessary due to bleeding from the surgery. There are two methods of transfusion, allogeneic transfusion (transfusion with the blood product of Japanese Red Cross Society) and autologous transfusion. Autologous transfusion is a method of transfusion where your blood is collected in advance one to two weeks prior to the surgery, and this blood is transfused during the surgery. There are cases where autologous transfusion is not possible due to anemia.
Progress During Hospitalization
The period of hospitalization is 10 to 14 days. The goal is to be able to walk with a cane.
Surgery
On the day of the surgery, you will go from your hospital room to the operating room. The anesthesiologist will administer your anesthesia and monitor you during surgery. The surgery will take around one hour. After surgery, we will confirm that you are in stable condition, and you will return to your hospital room.
Pain
After surgery, we will control the pain as much as possible. We will use a device that allows you to adjust the dose of painkiller according to the intensity of the pain.
Surgical Incision
Four to five days after surgery, when the incision appears dry, you will be able to take a shower.
Physical Therapy
A physical therapist will guide you in exercising your hip joints and practicing daily movements. You will begin to practicing walking holding on to parallel bars. Ordinarily, you will be able to walk with a cane after about one week. Physical therapy progresses differently for each individual.
Surgical complications
Infection (purulence)
The rate of incidence of deep infections of the surgical incision is approximately 1%. If a deep infection occurs, an extended period of time will be required for treatment. A repeat surgery may also be required.
Deep Vein Thrombosis/Pulmonary Embolism
There are cases where clumps of blood (blood clots) form in the veins of the lower limbs after surgery, causing pain and swelling in the legs (deep vein thrombosis). In rare cases, the blood clot may move inside the blood vessels and clog the blood vessels in the lungs (pulmonary embolism). A severe pulmonary embolism may result in death. In order to prevent thrombosis, a device that intermittently places pressure on the lower limbs or a medication that makes it slightly harder for the blood to clot (anticoagulant) is used.
Dislocation of Artificial Joints
If forced into a difficult position, the ball of the artificial joint may fall out of the socket and become dislocated. The rate of dislocation is several percent. The risk of dislocation is particularly high for approximately one month after surgery. Once the muscles recover after a certain length of time has passed after surgery, there is no need to particularly restrict your movements in your daily life.
Total Knee Arthroplasty
- About artificial knee joint replacement surgery
- About the department’s total knee arthroplasty (TKA) About minimally invasive surgery (MIS)
- About the department’s uni knee arthroplasty (UKA)
- About the department’s track record
- About simultaneous bilateral surgery
- About loosening and repeat replacement surgery
- About preparing for surgery
- About complications and risks
- About postoperative progress
- About life after being discharged from the hospital
- About fees
- How to book a consultation with the department
About Artificial Knee Joint Replacement Surgery
Artificial knee joint replacement surgery came to be widely conducted around the world in the 1980’s for joint diseases, and with the later development of new materials used in artificial joints and the improvement of surgical methods, the surgery is now being conducted around the world. It is also a common treatment method in Japan, with more than 80,000 surgeries conducted annually*. Artificial knee joint replacement surgery is conducted as treatment for knee joint disorders due to diseases such as osteoarthritis and chronic rheumatoid arthritis, and it alleviates pain in the joints, making it easier to walk, and is expected to improve the quality of life. Artificial knee joint replacement surgery consists of total knee arthroplasty (TKA) (photograph 1) and unicompartmental knee arthroplasty (UKA) (photograph 2). TKA is a surgery where both the femur and tibia and the joint side of the kneecap are replaced with artificial components. The femoral and tibial joints are replaced with strong metals such as titanium and cobalt-chromium alloy or ceramic, while a polyethylene component is attached to the tibial side. With UKA, only the inside of the femur and tibia are replaced.
*As of February 2025
Artificial Joint Registry Survey Report 2022 by the Japanese Society for Replacement Arthroplasty
“2022 Annual Report on the Joint Replacement Registry Survey”

[photograph 1]

[photograph 2]
About the Department’s Total Knee Arthroplasty (TKA)
The surgery is conducted using minimally invasive surgery (MIS) techniques. A 10 cm to 15 cm vertical incision is made on the front of the knee, and the deformed areas are replaced with artificial joints. The surgery will take around 1.5 hours. If you have a large build or strong deformity, the incision may become longer, and the time required for surgery may lengthen. If the surgery progresses as planned, the incision on the skin should be around 10 cm, and the surgery should be complete within one hour. If the knee has a strong deformity or if there are complications, the incision on the skin may lengthen to around 15 cm and the surgery may take more than two hours. The time required for surgery is the time from when the anesthesia takes effect and you become stable, after which preparations such as sterilization will be completed, then an incision will be made in the skin, and finally the skin will be sewn together. Anesthesia will be given around this time, and time is required for the anesthesia to stabilize and to gather the equipment. You will be monitored in the operating room after surgery until the anesthesia wears off and you are stable. The equipment models that are mainly used in the department have not only been approved by the Ministry of Health, Labour and Welfare (MHLW) in Japan, but also by the FDA, the US equivalent of the MHLW. The FDA approval standards are among the strictest standards in the world. We have selected a standard model that has achieved stable results in the US, Japan, and Europe (photograph 1). A deep flexion compatible model in line with the Japanese lifestyle has been developed, and is used by the department.
About the department’s unicompartmental knee arthroplasty (UKA)
UKA is indicated when conservative treatment such as medication and foot plates are not effective, and the cartilage and ligaments are not damaged to such an extent as to indicate TKA. Only the interior of the knee joints is replaced using MIS techniques.
About Simultaneous Bilateral Surgery
If there is strong deformity on both the left and right sides and there is significant damage, artificial knee joint replacement surgery may be conducted on both sides with one surgery. There are cases where it is only conducted on one side and the opposite side is done again, however, as only the deformity in one knee would be corrected while the opposite side would remain the same, the length of the legs would be different, leading to a leg length discrepancy that may slow the progress of physical therapy. If both sides are simultaneously operated on, physical therapy will progress smoothly. Of course, if you wish to operate on one knee at a time, the timing can be adjusted to conduct the surgeries as two surgeries. If conducting surgery on both sides simultaneously, the surgery will be more invasive, placing more stress on the body, and the feasibility of surgery needs to be determined upon considering complications, age, and stamina.
About Loosening and Repeat Replacement Surgery
TKA is a surgery with stable results. In most cases, the pain in the knees is alleviated over an extended period of time, and walking becomes easier. However, with regards to the flexion of the knee, even with the latest deep flexion compatible model, sitting on their heels in the traditional Japanese seiza style may be difficult. This is because even with the enhanced capabilities of artificial joints and a design that enables deep flexion, the muscles around the knee joint and the soft tissues such as the tendons have deteriorated and cannot withstand sitting on their heels in the seiza position. In addition, if you do not do very much physical therapy, the knee may become stiff before it bends. With time, artificial joints may loosen between the bone and metal. Currently, with the advances made in technology and the development of materials, the artificial joints themselves are designed to work without any issues for around 10 years after surgery, and they are beginning to function for even longer periods of 20 to 30 years. However, when accompanied by a disease that progressively destroys bone such as rheumatism, this long-term durability does not apply.
About Preparing for Surgery
Once you have decided to undergo surgery, began preparing for surgery as follows.
[Assessment of Your Physical Condition]
In order to examine whether it is possible for you to undergo the surgery, preoperative tests will be conducted within four weeks of the scheduled surgery. Tests such as a blood test, urine test, electrocardiography, and chest X-ray will be conducted. If the test results are abnormal, further testing may be required to examine whether surgery is feasible, you will be asked to consult a specialist.
[Comorbidities and Prescriptions]
If you have a disease for which you are being treated at another hospital, confirm information such as the name of the disease, treatment, and prescriptions with the physician you are consulting. Some medications may need to be discontinued or have their dosage adjusted prior to the surgery.
[Autologous Blood Deposit]
Ordinarily, even if autologous blood deposit is not conducted, there are cases where transfusion is not required. If there is extensive bleeding after surgery and anemia progresses, an allogeneic transfusion (transfusion with the blood product of Japanese Red Cross Society) will be conducted. For your peace of mind, an autologous blood deposit can be conducted upon request.
About Complications and Risks
TKA is certainly not a small surgery, but it is currently a sufficiently safe surgery. In spite of this, it is important to be aware of the complications and risks that may occur, such as infection (purulence), venous thrombosis, pulmonary infarction, and dislocation of the artificial joint.
- When infection (purulence) occurs in artificial joints, it often requires an extended period of treatment to heal, and we will pay close attention to ensure that infections do not occur. To ensure that an infection does not occur in the surgical incision, the surgery will be conducted in a sterile operating room, and preventive antibiotics will be administered.
In addition, if dental caries or athlete’s foot is left untreated after artificial joint surgery, the infection may spread to the artificial joints, and early treatment is recommended. - Blood clots may form within the venous blood vessels. This is called thrombosis, and after surgery, you will wear a device that continuously places pressure on the backs of the feet to prevent the formation of blood clots. When bleeding from the area that was operated on stops, we will use an antithrombotic drug that is eligible for insurance coverage. Elastic stockings will also be used. When a blood clot forms, the blood clot may circulate throughout the body and lead to pulmonary infarction and pulmonary embolism. If pulmonary infarction or pulmonary embolism occurs, it often becomes more severe, bur fortunately, we have never had a case with our artificial joint replacement surgeries where a pulmonary infarction or pulmonary embolism became more severe. If a pulmonary embolism does occur, it will be treated in collaboration with the General Medicine, Cardiovascular Medicine, and Respiratory/Pulmonary Surgery.
About Postoperative Progress
The surgical incision ordinarily heals after approximately two weeks. The incision will be quite painful for two to three days immediately after the surgery, but the pain will be alleviated using a device that continuously injects painkillers. After surgery, your knee will be bent and straightened using a device called a CPM, and a physical therapist will conduct physical therapy to acquire muscle and bend the knees. When the condition of the knees improves, you will practice standing up and walking, and after two to three weeks of hospitalization after the surgery, you will be able to walk with a cane and can be discharged. If simultaneous bilateral surgery was conducted, you will be able to walk with a cane after three to four weeks of hospitalization and can be discharged. Compared to just one side, hospitalization will be extended approximately one week. If it takes more than four weeks after the surgery to be able to walk with a cane, or if you wish to have additional physical therapy even after you are able to walk with a cane, you may be transferred to a rehabilitation hospital for physical therapy.
About Life After Being Discharged From the Hospital
You will gradually acclimate to daily life. It will take from three to six months to acclimate. With conventional models, there were cases where it was difficult to stand on the knees, but with the deep flexion compatible model, you should be able to stand on your knees.
Artificial joints are just “artificial” joints, so even if the pain is gone, you will damage the joints early on if you move too violently or expose the limbs to strong impact, causing the joints to loosen.
About Fees
Health insurance, long-term care insurance, and various systems such as eldercare may be utilized to decrease the financial burden of the fees for artificial knee joint surgery. In the hospital’s General Counseling Center, a social worker will help you investigate what systems can be used. If health insurance is used without completing the procedures for the various systems, you will pay the 10% or 30% co-payment, but by applying to use the High-Cost Medical Expense Benefit, your co-payment will be adjusted according to your income.
Reverse Total Shoulder Arthroplasty
The rotator cuff is composed of four muscles that stabilize the inherently unstable shoulder joint from within. Due to this internal stabilizing function, these muscles are commonly referred to as the “inner muscles” or “inner unit”. In contrast, the deltoid muscle, known as an “outer muscle”, serves as the main driving force for shoulder movement. However, the deltoid functions properly only when the rotator cuff is intact (Figures 1 and 2). When the rotator cuff is torn—especially in large or massive tears—the patient may lose the ability to lift the arm. In such cases, surgical reconstruction is often necessary to restore shoulder function. Reverse total shoulder arthroplasty (RTSA) is a surgical procedure that allows for functional recovery of the shoulder joint even in the absence of a functioning rotator cuff. This technique has been available in Japan since 2014, and our institution adopted it in 2019. Below, we describe the surgical procedure in more detail.
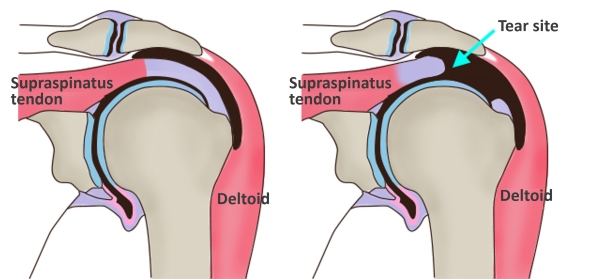
【Figure 1, 2】
Indication:This procedure is indicated for massive and irreparable rotator cuff tears. When the tear size becomes large, it may prevent the humeral head from maintaining its centered position (loss of humeral head centering), which can result in an inability to elevate the upper limb. These cases represent the most appropriate indications for surgery.
Surgical Method
The shoulder joint functions based on a ball-and-socket relationship. The reverse total shoulder arthroplasty is so named because it reverses this relationship in the artificial joint. Figure 3 shows a standard total shoulder arthroplasty, while Figure 4 illustrates a reverse total shoulder arthroplasty. By reversing the ball-and-socket configuration, the stability of the shoulder joint is improved, allowing elevation of the arm using only the deltoid muscle (an outer muscle), even in the absence of the rotator cuff. A skin incision of approximately 10 cm is made on the anterior aspect of the shoulder, and the surgery typically takes around 1 hour and 30 minutes. Blood transfusion is rarely required.
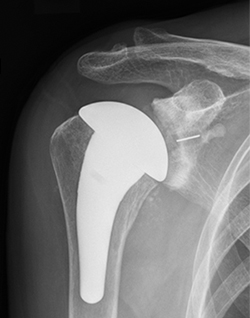
【Figure 3】
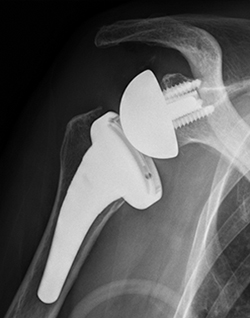
【Figure 4】
Life After Surgery
After surgery, rehabilitation is essential to restore the range of motion. About three months after the procedure, patients can typically resume moderate activities such as jogging, golfing, or hiking. Since artificial joints have a limited lifespan, high-impact activities are not recommended in order to extend their durability.
Durability of Artificial Joints
With advancements in materials and technology, the durability of artificial joints has improved. However, over time, wear and loosening between the joint and bone can occur, which may require revision surgery to replace the artificial joint.
Hospital Stay
The typical hospital stay is about 7 to 10 days. Patients will wear a brace after surgery, and for those who live alone, an extended stay of about three weeks may be possible until the brace is no longer needed.
Surgery
On the day of surgery, you will be transported from your hospital room to the operating room. An anesthesiologist will manage anesthesia and monitor your overall condition during the operation. The surgery usually takes about 1 hour and 30 minutes. After confirming your stability post-operation, you will return to your hospital room.
Pain Management
Postoperative pain will be carefully managed through methods such as nerve blocks, oral medications, and IV pain relief to ensure your comfort.
Surgical Wound
You may begin taking showers around 3 to 4 days after surgery, once the surgical wound has dried.
Rehabilitation
A physical therapist will guide you through shoulder joint exercises and daily living activities. The pace of rehabilitation varies from person to person.
Surgical complications
Infection:
Deep infections at the surgical site occur in about 1% of cases. If this happens, long-term treatment may be needed, and revision surgery may be required.
Dislocation of the Artificial Joint
Dislocation can occur if you move into an unnatural or extreme position. The risk of dislocation is about 1%. The risk is particularly high during the first month after surgery. Once a certain amount of time has passed and muscle strength has recovered, there is generally no need to restrict daily activities due to fear of dislocation.
Fractures:
Fractures may occur during or after surgery. Overuse of the affected limb too soon after surgery increases this risk. Avoid heavy labor or strenuous activity for at least three months following surgery.
How to Book a Consultation With the Department
This department is by appointment only. Please prepare a referral from your primary care physician and make an appointment for a consultation through the hospital reservation center. Please refer to the hospital website for details.
Director Hirofumi Oshima